TENDON PAIN
Tendinopathy (tendon pain) is very common. They are the most common type of overuse injury (ref). Achilles tendinopathy affects the majority of runners (ref) and is the reason 16% of athletes have to stop sports participation (ref).
There are a range of commonly prescribed treatment options for tendinopathy, but very few are supported by quality, randomised, prospective, placebo-controlled trials. SO WHAT DO I DO?
Considering all the available treatment options, above anything else, I always recommend:
WHAT ABOUT INJECTIONS?
Having mapped out a management plan, patients will routinely ask my opinion on getting an injection. They may have had a friend for whom an injection worked well, or the GP has suggested it as an option, or they’ve had one before and it worked.
There are a range of drugs to inject into or around a tendon, depending on who you are referred to:
CORTICOSTEROIDS
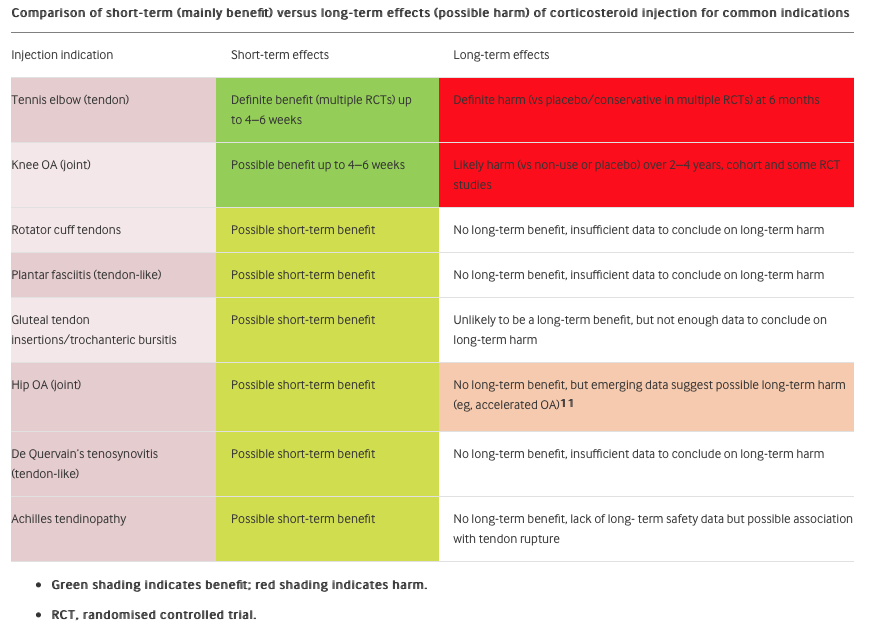
Corticosteroids are an anti-inflammatory medication injected around the tendon to decrease pain that is caused by inflammation (although it is now thought that inflammation does not play a significant role in tendon pain). Corticosteroid injections have historically been commonly prescribed but more recently their use is controversial. Repeated corticosteroid injections can weaken the tendon and increase the risk of rupture. Corticosteroid injections are good at relieving pain in the short term (2-6 weeks) however, there is strong evidence that long-term outcomes (> 6 months) are worse than other conservative treatments or no treatment at all (ref).
"The best systematic review evidence shows that local corticosteroid injections are not effective for tendinopathies after the first few weeks, and produce worse long-term outcomes compared to other treatments" (ref) PROLOTHERAPY / SCLEROTHERAPY
Prolotherapy injections act as an irritant causing an inflammatory response then scarring of the nerves that transmit pain. There is no solid support in the medical literature for this procedure for the treatment of tendinopathies. A randomised controlled trial of polidocanol injections showed the potential to reduce tendon pain in patients with chronic painful mid-portion Achilles tendinopathy (ref). However, a systematic review found limited results for use of prolotherapy in sports related soft tissue injuries (ref).
AUTOLOGOUS BLOOD INJECTIONS
The rationale of autologous blood injection consists of enhancing tendon healing through collagen regeneration and the provision of cellular mediators. Good experimental models are lacking, and clinical application is anecdotal. A 2013 randomised controlled trial investigating the efficacy of autologous blood injections as a treatment for mid-portion Achilles tendinopathy concluded they did not reduce pain or improve function any more than a strengthening program. (ref)
HIGH-VOLUME INJECTIONS
The suggested mechanism of high-volume injections is the mechanical disruption of local tissues then stimulates a healing response. One study (ref) has shown that high-volume injection of normal saline solution, corticosteroids or anaesthetics reduces pain and improves short and long-term function in patients with Achilles tendinopathy. However, more research is required.
PLATELET RICH PLASMA (PRP)
Platelets are naturally occurring in your blood, where they play an important role in healing damaged tissue, so superficially it’s inherently appealing to just add more of them to the sore spot. PRP injections are particularly trendy at the moment and it’s easy to find someone who will tell you they work well. Unfortunately, research concludes there is no benefit to PRP injections. This study found PRP injections do not improve plantar fasciopathy pain or function. This study concluded there is insufficient evidence to support the use of PRP for treating musculoskeletal soft tissue injuries. This systematic review found strong evidence against platelet-rich plasma injections for tennis elbow. This study found PRP did not improve tendon structure. This meta-analysis found no greater clinical benefit of PRP over placebo or dry needling for tendinopathy.
SO…
Would I have any of these injections, or would I recommend them to my patients, friends, or family? Well it depends. In my experience some people get some benefit some of the time. HOWEVER, these injectables are not consistently effective and their use is mostly not supported by research. I suggest that patients try the strengthening program and the results will be overall better in the long term.
WHY DO THE INJECTIONS WORK FOR SOME PEOPLE?
I’ve been frustrated with a couple of patients that cancelled their follow-up appointment and, when I phoned and asked what had happened, they’ve had an injection and now feel fine. My conclusion is the injections don’t work, but if you were sore and now you’re not, your conclusion would be they do work. So what is it?..
REGRESSION TO THE MEAN
Most people seek treatment when they are at their worst. By definition the only possible change from being as bad as at can be, is an improvement. Was it the injection working, or was it getting better anyway?
NATURAL HISTORY
Some conditions are self limiting and will just get better by themselves. Did the injection work, or was it about to get better anyway?
PLACEBO
SUMMARY
I understand that getting an injection seems like a much easier option than doing 12-weeks of strengthening exercises, but in the long run, a strengthening program is the thing that actually works.
TL;DR
If treating tendon pain was as easy as getting an injection then that’s what everyone would do first. Unfortunately it’s not as easy as that.
I treat a lot of people that have:
Very commonly they’ll tell me something is “out of alignment”. Either that’s what it feels like, or they’ve had treatment from a therapist that has told them that, or they’ve talked to a friend who has said “maybe your ‘X’ is out?” and that makes perfect sense to them. The concept of something being “out of alignment” is not a paradigm I’ve ever been taught or taught to patients. My understanding of it as an idea is that it comes from an osteopathic and chiropractic model where pain and illness are meant to originate from vertebral “subluxations”. A vertebra is “out of place”. The subluxation model is now being discouraged by chiropractic associations worldwide as not being valid, but it has definitely seeped into public consciousness. A lot of people when they have back pain will try and describe how it feels and come up with the explanation that they’ve “put their back out”. Patients grab hold of a simple idea that seems to makes sense. When a patient uses this sort of terminology I used to play along with it because I understood what they were saying and I found I upset a lot of patients if I tried to correct them. They had paid good money to see a chiropractor who’s told them their pelvis was out of alignment, they’ve agreed that’s what it felt like so they’ve bought into the idea. When I question the concept directly it can be upsetting. If someone to whom you’ve paid money tells you something, and they’re a nice enough person, and they seem like they care about you and know what they’re talking about, you believe them. To then be the second therapist offering an opinion and say something different can be tricky and I usually word it incorrectly and put the patient right off side.
Anyway, I used to let it slide because it’s easier for everyone, I can get on with treatment using my own paradigm, and I didn’t think any harm was done.
But I’ve now changed my mind on staying quiet. I saw a lady today who’s been seeing an osteopath twice a week for a year - thousands of dollars - for a radiculopathy from her lumbar spine which has now progressed to a foot drop. Every session her “pelvis was out”. She doesn’t know how it keeps happening. Her only solution was to pay this “expert” for a “re-alignment”. It’s a very common story. I got so upset today. This lady was in tears - she felt so helpless. I think this sort of treatment is criminal. It makes someone a helpless victim by diagnosing them with something that they have absolutely no control of themselves - the pelvis just keeps going out mysteriously. And sell a solution: “I can put it back for you. Come in twice a week”. Nothing you can do to help yourself. The language is dangerous and damaging and takes advantage of a patient that trusts you are a professional providing an honest service. When a therapist talks about something being out of alignment I hope they are using the terminology as a euphemism rather than believing something is actually out of place. Because we know it’s not. So the therapist is either:
So I’m no longer tolerating the language of something being out of place or out of alignment.
|
�
Archives
July 2024
Categories
All
|
|
|
MENU
|
INJURY INFO
|
INJURY INFO
PHYSIO MOSMAN |
Copyright© 2024| Fit As A Physio | ABN 62855169241 | All rights reserved | Sitemap



 RSS Feed
RSS Feed